
Plan sponsors see the value in improving member access to care for improved health outcomes—with key actions that help drive down the total cost of health care. But how can health plan administrators make the informed choices that help influence those key actions?
Health care costs are anticipated to inflate in 20221 for several reasons, including:
- The lingering impact of COVID-19 on the medical system, as those who have delayed care are now seeking it.
- The ongoing crisis of mental health care and substance abuse.
- An overall decline in general population health.
Shift in consumer behavior
Conversely, we are seeing health care consumer behavior shifting, as members lean in to lower-cost and more convenient sites of care. Emergency rooms are becoming a last resort for members seeking non-emergent care, where more accessible options have proliferated. Choices such as digital and virtual options have become a welcome relief from time spent in a crowded waiting room.
Within our own business, we witnessed a 42% drop in emergency room visits during the March to April lockdowns of 2020, but a resulting shift in behavior that with overall emergency room visits down 25% compared to pre-pandemic levels.
Investments in lower-cost site of care solutions, including digital and virtual options—and the immediate surge of adoption from members—may initially increase spending. But the short- and long-term savings projections are impressive, and help prove these plan additions add to value for plan sponsors and members.
Solutions that impact care and boost savings
Point solution options for digital and virtual care—products and services that give members access to the care they need when they need it—have rapidly expanded. These not only service urgent need, but provide disease-specific and general medical options for affordable access points that help plans mitigate primary cost drivers. While we expect to see an increase in investment and plan sponsor spending on these tools, the resultant savings have already proven significant on a simple premise: more personal, coordinated care. This ultimately increases the likelihood of engagement, raising access rates.
Hinge Health: driving down the cost of musculoskeletal conditions
- Reported outcomes show (Graphics)60 percent fewer surgeries needed
- 50 percent drop in pain and depression
- Big boosts in member satisfaction rates
- Overall 1.5:1 ROI
The total cost of care is further lowered when benefit designs favor both quality and accessibility. Navigation partnerships are often a beneficial layer, supporting member decision making. Additionally, benefit plans should reflect an emphasis on social determinants when evaluating plan design and solution choices.
In a market where point solutions proliferate, national health plans are increasingly creating rigid, aggregated plans and endangering real flexibility, Meritain Health provides options… options to do what the plan sponsors want and need.
Meritain Health offers a unique space
Meritain Health has carved a unique space with our ability to provide what other TPAs cannot offer. As a wholly owned subsidiary of CVS Health and Aetna, Meritain Health retains its TPA DNA, defined by ultimate flexibility, while developing and curating the very best solutions from CVS, Aetna and the market as a whole. We refer to this concept as
Meritain Connected Solutions.
Specifically, Meritain Connected Solutions offers:
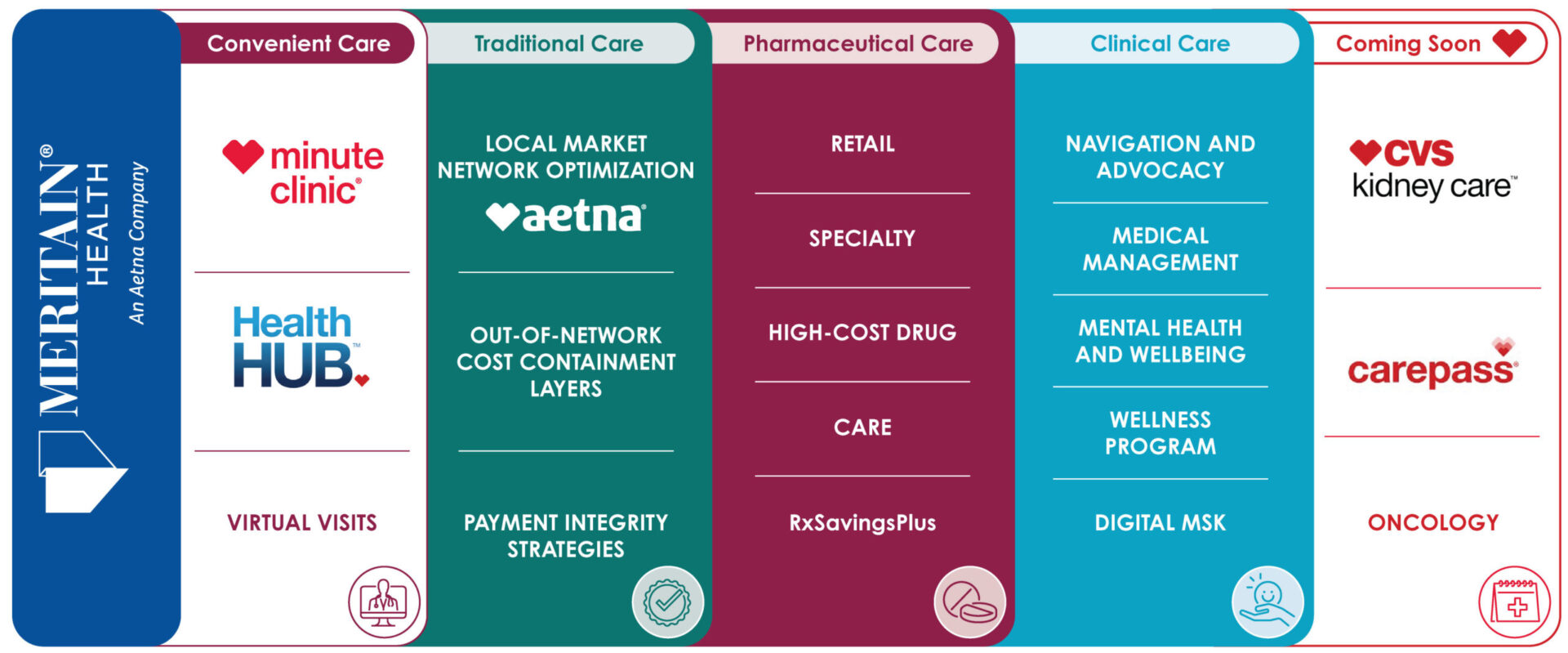
Layering solutions that meet the needs of our customers, we bring forward the best options toaddress the most critical cost drivers, while evolving based on market need and feedback. We carefully review the needs of each plan sponsor and draw from our vast pool of products and services to connect our customers with the solutions that deliver the most value to their plan. This includes available offerings from CVS and Aetna, and our wide array of point solutions and vendor partnerships.
Within Meritain Connected Solutions we’ve created an Integrated Value Guarantee, a promise on how utilizing specific combinations of solutions will demonstrably lower claims spend.
Contact us today to learn more about how Meritain Health can lower your total cost of care through Meritain Connected Solutions and our Integrated Value Guarantee.
About Meritain Health
As Advocates for Healthier Living, we’re improving clinical outcomes while reducing the Total Cost of Care. We help our clients combine our plan administration and external point solutions with the right products and services from Aetna and CVS Health. For more information, contact your Meritain Health representative.
1 PwC Medical cost trend: Behind the numbers 2022



